Neurology
Browse our resources, designed to help you stay up to date on emerging treatments and the latest disease management strategies.
Medical conditions
ADHD
Latest news, insights, and guideline updates
CIDP
Latest updates on diagnosis and management
Dementia
Latest news, insights, and guideline updates
Depression
Disease information, latest news, and guidelines
Epilepsy
Latest news, insights, and guideline updates
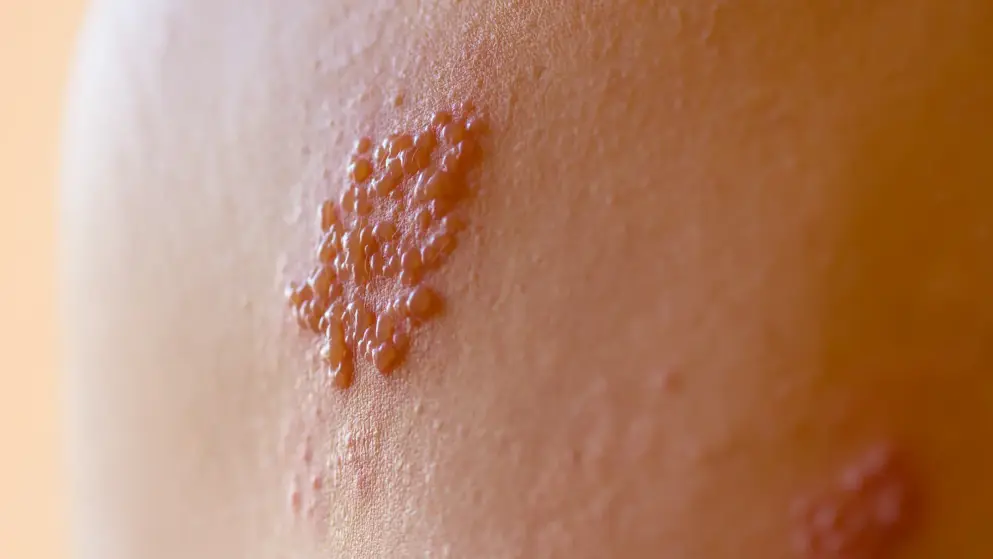
Herpes zoster
Test your knowledge with our quick quiz
Migraine
Latest insights and spotlight article
Multiple sclerosis
Risk factors, epidemiology, and treatments
Myasthenia gravis
Case studies, podcasts, and congress highlights
Pain
Latest insights and spotlight articles
Parkinson’s disease
Latest insights and spotlight article
Pompe disease
Patient insights and expert guidance
TK2d symposium
Gain expert insights into diagnosing and treating thymidine kinase 2 deficiency in pediatric patients.
Latest resources
Accredited symposium: Elevating LOPD care
Watch Benedikt Schoser and colleagues discuss unmet needs in LOPD and how new patient insights are informing clinical practice and improving outcomes.
Myasthenia gravis at EAN 2024
Read about myasthenia gravis at the European Academy of Neurology (EAN) Congress 2024 in this three article series covering personalised treatments, the impact of sex on MG outcomes, and emerging treatment options for MG, including complement inhibitors and neonatal fragment crystallisable receptor (FcRn) blockers.
Exercise for treating Parkinson’s disease
This short article reviews the role exercise plays in reducing the risk of Parkinson’s disease, and in improving motor symptoms associated with the disease.
Browse older resources
Anti-CGRP Therapies for Migraine
Learn about unmet needs and disease burden associated with migraine, the role of CGRP in its pathophysiology, and anti-CGRP therapies for acute and prophylactic treatment of migraine.
Major Depressive Disorder & Treatment-Resistant Depression
The treatment landscape for major depressive disorder (MDD) and treatment-resistant depression (TRD) is evolving, with recent approvals impacting on treatment algorithms.