Medical education
Accredited CME for continuing professional development
Accredited HLH/MAS masterclass
Diagnosing and treating HLH/MAS: Earn 1 CME credit
Accredited symposium: Elevating LOPD care
Join Prof. Schoser, Dr. Mozaffar and Dr. Kishnani for an accredited symposium focused on translating patient perspectives into effective care.
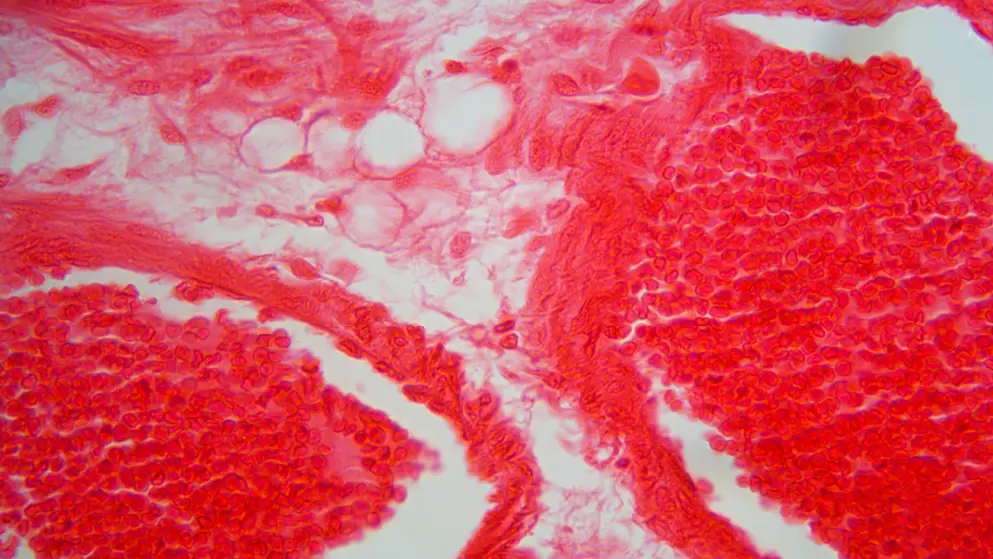
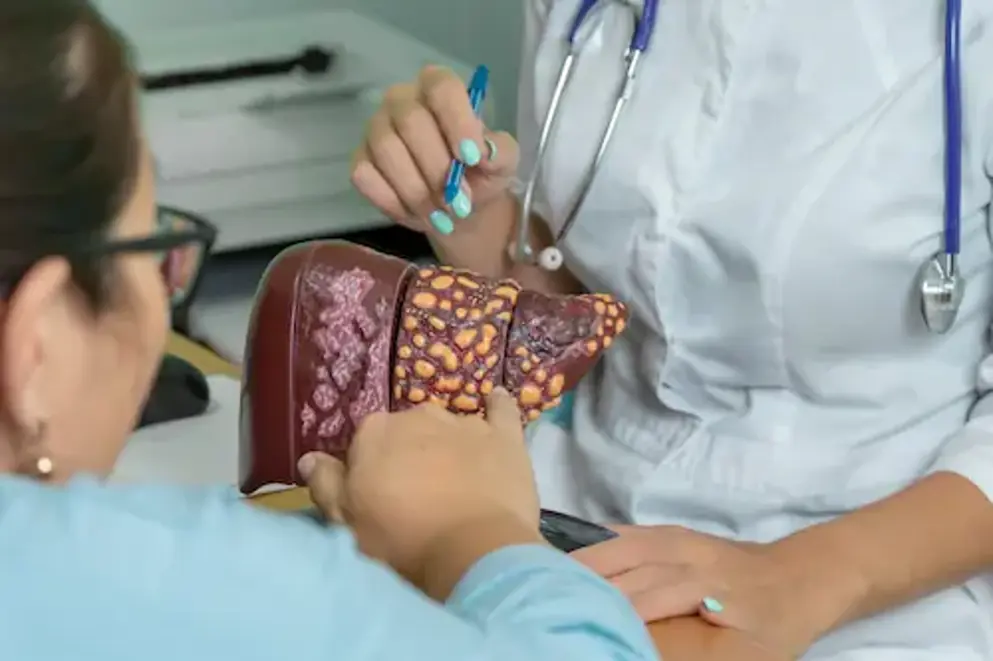
Alpha-1 antitrypsin deficiency
Expert insights on AATD-associated liver disease
Podcast: Understanding AATD
Listen to expert discussions and earn 1.5 credits
Learning Zones
Alpha-1 antitrypsin deficiency
Expert insights on AATD-associated liver disease
HLH/MAS: A multifaceted syndrome
Take our accredited masterclass
Expert insights on CSU management
The latest in CSU diagnosis and care
Chronic Inflammatory Demyelinating Polyneuropathy
Gain a comprehensive overview of CIDP, including diagnostic challenges and how to apply the latest guidelines in practice.
Managing High-Risk NMIBC
Expert and patient insights on high-risk NMIBC, including relevant clinical trial data and standout congress sessions.
HRR mutation testing in mPC
Updates in HRR gene testing in mPC
Advances in HS
EHSF 2024: Surgical updates and changes to practice
mCRPC in Focus
Unmet needs in the management of mCRPC, with a focus on treatments
Think Thrombosis
Latest data and clinical guidance
Advances in Lymphoma
Information on current lymphoma care and treatments for classic Hodgkin lymphoma (cHL), PTCL subtypes, relapsed DLBCL, and B-NHL.
Alopecia areata: Progressing practice
Latest treatment options and patient insights
Myasthenia Gravis Learning Zone
Medical education resources focused on identifying early symptoms of myasthenia gravis, available treatments and information about the latest findings in new therapy pathways
Anti-CGRP Therapies for Migraine
Learn about unmet needs and disease burden associated with migraine, the role of CGRP in its pathophysiology, and anti-CGRP therapies for acute and prophylactic treatment of migraine.
Antiplatelet Therapy in ACS: Choices and Controversies
Acute coronary syndrome (ACS) represents a leading cause of mortality and morbidity worldwide. Antiplatelet therapy is a cornerstone of ACS management.
CDK4/6 Inhibitors in Breast Cancer
Are you familiar with the clinical trial evidence that could help you to select the best cyclin dependent kinase 4/6 (CDK4/6) inhibitor for your metastatic breast cancer patient?
Chronic Kidney Disease Learning Zone
Chronic Kidney Disease (CKD) is a disease that can often lead to a need for haemodialysis and kidney transplantation. New CKD treatments are emerging which focus on delaying CKD disease progression and the need for transplantation.
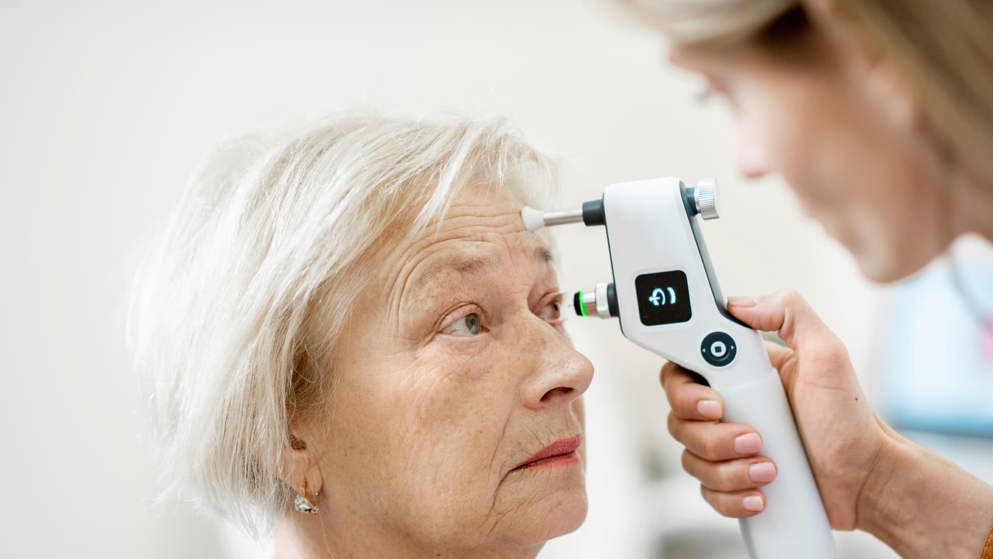
Glaucoma Learning Zone
Learn more about risk factors and symptoms of glaucoma, watch expert videos on glaucoma screening and diagnosis, and test your knowledge of glaucoma treatments with a series of patient case studies and quizzes.
Growth Hormone Deficiency
An introduction to growth hormone deficiency (GHD), summarising the content. A quiz on GHD, followed by links to pages on GHD symptoms, diagnosis and treatment landscape.
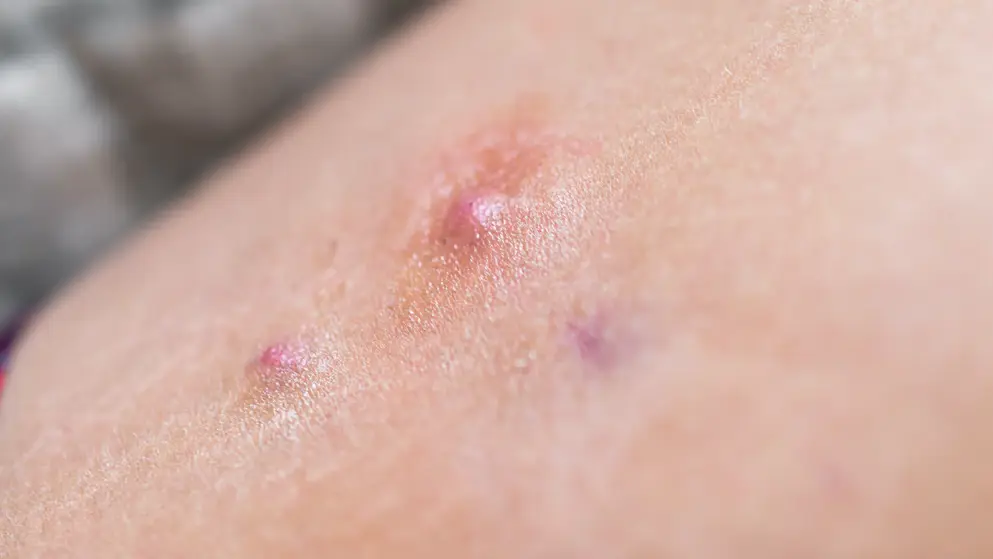
Hidradenitis Suppurativa Learning Zone
Explore updates on diagnosis, epidemiology, disease burden, pathophysiology, and future treatments for HS.
Lupus Learning Zone
Systemic lupus erythematosus (SLE) is a highly burdensome disease, with the worst affected SLE patients suffering refractory disease and organ damage accrual.
Multiple Sclerosis (MS) Learning Zone
Choosing the right treatment is critical to managing multiple sclerosis (MS). Consider your options with the latest data from over 40 MS clinical trial and congress resources.
Pompe Disease: Key findings from WMS 2022
Review developments in Pompe disease, expert opinion and discussion, and more in the following pages. Highlights and forthcoming expert content focus on the 2022 World Muscle Society Congress which was held in Halifax, Canada 11–15 October.
Psoriasis Academy
When it comes to psoriasis, a knowledgeable healthcare professional is highly valued by patients (Pariser et al., 2016). With this in mind, we created The Psoriasis Academy, an online hub featuring succinct and easily accessible information for all healthcare professionals who want to know more about psoriasis and keep up to date with the latest developments.
Supportive Care in Oncology Learning Zone
Supportive care in oncology from a multidisciplinary team involves caring for patients with cancer, treatment adherence and adverse effect management.
Ulcerative Colitis Learning Zone
Explore the role of biologics and targeted small molecules in UC management, and listen to expert insights on integrating them into practice.
Roundtable: Biologics in plaque psoriasis
Watch expert roundtable on the use of biologics in moderate-to-severe plaque psoriasis, chaired by Professor Luis Puig.
Introducing vasomotor symptoms
Vasomotor symptoms (VMS) remain one of the most impactful aspects of menopause.
Learn more about their impact and the treatment options available with "VMS breakthroughs" a 4 article series focused on VMS
Myasthenia gravis at EAN 2024
Read about myasthenia gravis at the European Academy of Neurology (EAN) Congress 2024 in this three article series covering personalised treatments, the impact of sex on MG outcomes, and emerging treatment options for MG, including complement inhibitors and neonatal fragment crystallisable receptor (FcRn) blockers.
AL amyloidosis interactive patient journey
Make your own clinical decisions for managing a patient with AL amyloidosis in this interactive patient journey, guided by additional management tips provided by Dr. Shaji Kumar every step of the way.
HER2-low, PARP inhibitors, and more from SABCS 2022
Catch up on the latest developments in breast cancer from San Antonio with our coverage of SABCS 2022.