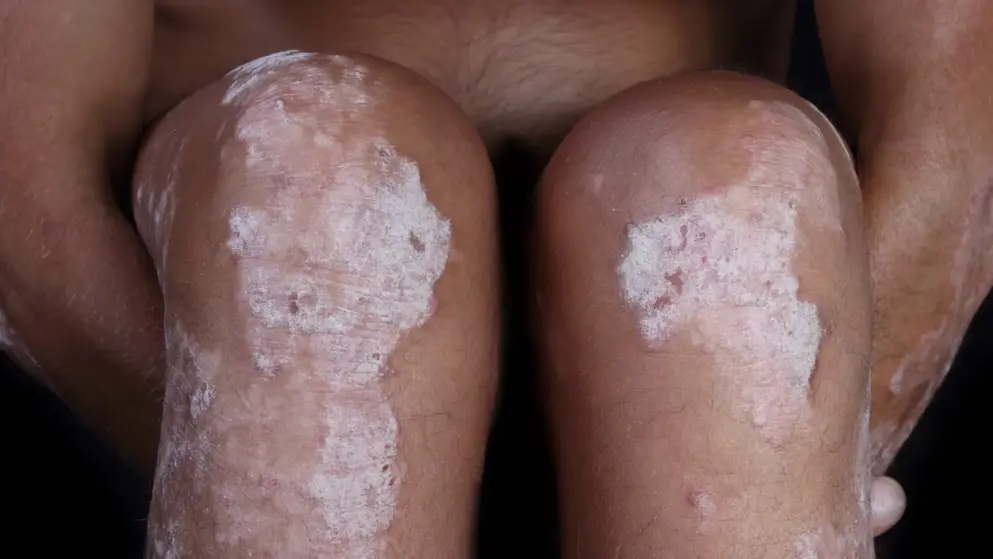
Moderate-to-severe psoriasis: treatment for young women
In part 1, Professor Diamant Thaçi, the director of the Comprehensive Center of Inflammation Medicine at the University of Lübeck, Germany, pointed out that young female psoriasis patients experience greater stigmatisation, lower levels of happiness, higher levels of stress and experience additional burdens related to family planning.
Here, Professor Thaçi expands on the key considerations when deciding how to treat this patient group at the outset, and which moderate-to-severe psoriasis treatments are proven to be safe in women who are of childbearing age (18–45 years).
At what point should physicians discuss family planning with women of childbearing age?
Professor Thaçi responds to the question ‘Is it important to discuss family planning early on?’
A key unmet need in young women is a lack of information and guidance on managing psoriasis, particularly if they are planning a family. There is evidence that women with psoriasis are less likely to become pregnant; however, have an equivalent chance of having an unplanned pregnancy. Given that treatments for moderate-to-severe psoriasis are not all suited for women who are pregnant or breast feeding, it is important for physicians to initiate the discussion on family planning early on with any young female patient, regardless of their intention to start a family. Not only is this important to guide treatment planning, it also informs the patient of their options at the outset so they can make better informed decisions.
Professor Thaçi highlights that early discussion with young women impacts on treatment planning.
Are there moderate-to-severe psoriasis treatments which are more suitable for young women?
The treatments currently available for moderate-to-severe psoriasis are not all suited for women who are pregnant or breastfeeding. This is partly related to known safety concerns, but also to the lack of evidence for safety in this patient group. Safety data for pregnant and breastfeeding women is most commonly sourced from registries that rely on observational input from physicians, since pregnant women are generally not included in initial clinical trials. For this reason, safety data is more robust in treatments that have been approved for longer, not just for moderate-to-severe psoriasis but also for other chronic inflammatory indications. Follow-on clinical trials that specifically address pregnant or breastfeeding women provide an even stronger basis for safety in this patient group.
Of the biologic treatments for moderate-to-severe psoriasis, only TNF-α inhibitors have been approved long enough to gather meaningful data on safety in pregnant and breastfeeding women. Clinical trial safety data for TNF-α inhibitors include the recently published prospective CRIB and CRADLE clinical trials on certolizumab pegol that show no to minimal transfer through the placenta and breastmilk. These findings offer confidence in biologic treatments for this patient group, for whom TNF-α inhibitor treatment is typically discontinued following the first trimester to limit placental transfer of the drug.
We ask Professor Thaçi ‘There appears to be more safety data available in young women for TNF-α inhibitors. Does this mean that TNF-α agents should be preferred over other effective treatments?’ and ‘How important is the recent pharmacovigilance safety data for exposure to certolizumab pegol, as a known example of a TNF-α inhibitor?’
The CRIB and CRADLE clinical trials on certolizumab pegol
The only biologic treatment with clinical trial data for pregnancy and breastfeeding in its label is certolizumab pegol, a TNF-α inhibitor that was recently approved for the treatment of psoriasis (EMA, 2018), with its first EMA approval for rheumatoid arthritis in 2009. Placental transfer of maternal IgG is known to take place in the second and third trimesters and is mediated through the neonatal Fc receptor. Certolizumab pegol differs in structure to other TNF-α inhibitors, lacking the Fc fragment that mediates placental transfer, but retaining a humanised Fab’ fragment linked to two polyethylene glycol (PEG) molecules (Figure 1).
Figure 1. Structures for TNF-α inhibitors infliximab, etanercept, adalimumab and certolizumab pegol. CDR, complementarity-determining region; PEG, polyethylene glycol; TNFR, tumour necrosis factor receptor.
Professor Thaçi points out key structural features of certolizumab pegol that makes it suitable for use in pregnant and breastfeeding women.
In line with its structural design, the CRIB clinical trial (NCT02019602) found negligible plasma levels of certolizumab pegol in the umbilical cord and infants compared to that of the mothers who received either a two-weekly or four-weekly regimen of certolizumab pegol (infant/mother plasma ratio 0.0009)1. The pharmacokinetic CRADLE clinical trial (NCT02154425) showed that certolizumab levels were not measurable in 56% of breast milk samples (n = 137) taken from 17 similarly treated mothers2. The remaining samples had negligible certolizumab levels (Figure 2). Altogether, these data indicate that at least certolizumab pegol can be recommended for treating female psoriasis patients who are planning pregnancy or breastfeeding.
Figure 2. Results for the CRIB and CRADLE clinical trials for the TNF-α inhibitor certolizumab pegol in pregnant and breastfeeding women.
Concluding remarks
More data is needed to understand the safety of other modern biologics in treating pregnant and breastfeeding women with moderate-to-severe psoriasis, in line with studies produced for certolizumab pegol. The acquisition of data needs to come from carefully controlled clinical trials, but also registry data that requires the active participation from relevant healthcare practitioners. Indeed, professor Thaçi reminds us that it is important to control moderate-to-severe psoriasis in order to have the best outcome for both the mother and baby.
Join us next time for Part 3 where we will discuss biologic treatment options for patients who present with multiple psoriasis features and those who have failed on prior biologic treatment.
Further reading
1. Mariette X, Förger F, Abraham B et al. Lack of placental transfer of certolizumab pegol during pregnancy: results from CRIB, a prospective, postmarketing, pharmacokinetic study. Ann Rheum Dis. 2018;77:228–233.
2. Clowse ME, Förger F, Hwang C et al. Minimal to no transfer of certolizumab pegol into breast milk: results from CRADLE, a prospective, postmarketing, multicentre, pharmacokinetic study. Ann Rheum Dis. 2017;76:1890–1896.
3. Gottlieb AB, Ryan C, Murase JE. Clinical considerations for the management of psoriasis in women. Int J Womens Dermatol. 2019;5:141–150.