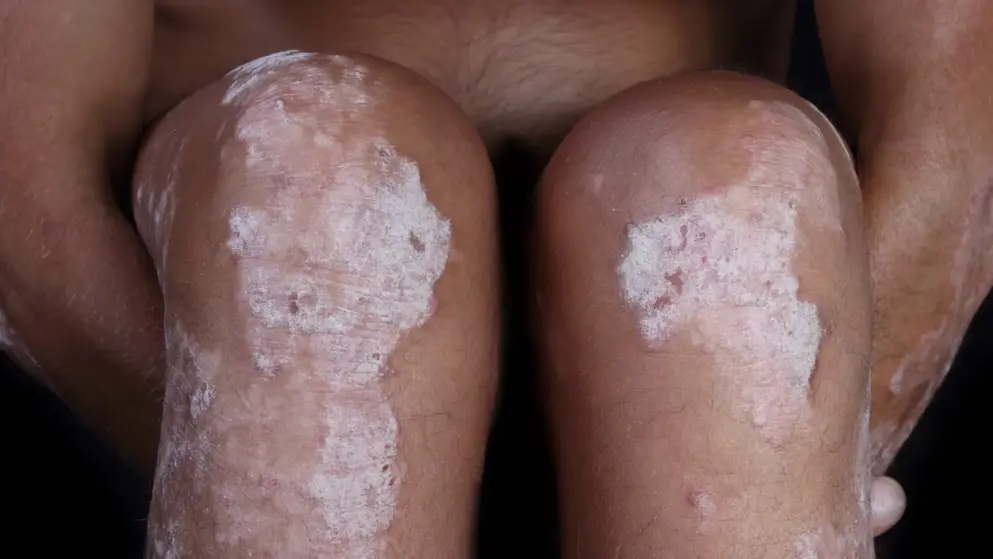
Moderate-to-severe psoriasis: the disease burden and unmet needs in different patient groups
In the subsequent parts, we will discuss:
Part 2: Treating moderate-to-severe psoriasis in young women of childbearing age
Part 3: Considering differences in the evidence base for moderate-to-severe psoriasis treatments
Throughout the series, we present key opinions from Professor Diamant Thaçi, the director of the Comprehensive Center of Inflammation Medicine at the University of Lübeck, Germany. Professor Thaçi’s work over the last 30 years includes both basic and clinical drug development studies for multiple chronic inflammatory skin disorders, including psoriasis.
Psoriasis
Psoriasis is a common chronic autoimmune skin disease, estimated to affect around 2–4% of the population in the Western world. For psoriasis, genetic factors interact with environmental aggravators such as stress and infections to produce varying degrees of disease severity and disease states, including plaque psoriasis, nail psoriasis and guttate psoriasis. Additionally, approximately 20% of psoriasis patients experience psoriatic arthritis (PsA) which differs in clinical management to skin-based disease.
Burden of disease
Psoriasis is associated with a high level of physical and psychological burden, triggered mainly by the presence of visible disfigurement of the affected skin. Psoriasis is most often characterised by well defined, infiltrated red plaques that form on highly visible areas of the body, including the elbows, knees and scalp, though it can affect any area of the body, including the nails and genitals. There is also a high physical burden related to itching, burning and bleeding of the affected skin. Burden of disease is further complicated by the presence of comorbidities such as psoriatic arthritis, metabolic syndrome, depression and cardiovascular disease.
Burden of disease in the young female population
Historically, patients seeking help for moderate-to-severe psoriasis were mostly between the ages of 40–50 years old. More recently, there has been a demographic trend toward younger patients seeking help and often, seeking fast solutions. Approximately half of these younger patients are women of child-bearing age that present burdens that are distinct to this patient group.
Professor Thaçi highlights that young women experience an indescribably higher burden of disease, irrespective of whether they are planning a family.
‘I think that in the female patients, that they really do suffer. It’s also the way how you look. It’s also the way how you have the first contact. It’s the way how you feel and we have a lot of patients (who suffer), even if they are accepted by their partners, their husbands and their friends…the stigmatisation is something that is really deep inside of this patient’.
This key point is reflected in the statistic that female patients with psoriasis are 50% less likely to have children compared to unaffected individuals. For younger women who are planning a family, the most common worry is on the safety of available treatments, particularly if they are systemic. These include worries on the impact of treatment on fertility, the unborn child during pregnancy, and breastfeeding a newborn child.
Professor Thaçi responds to the question, ‘Are your young female patients with psoriasis worried about whether psoriasis affects their fertility?’
Disease pathophysiology
Modern treatments for moderate-to-severe psoriasis are based on the pathophysiology of the disease. Psoriasis is a chronic immune-mediated disease that leads to cutaneous inflammation and keratinocyte hyperproliferation. Briefly, the initiation of a psoriatic state involves:
- The activation of dendritic cells via IL-1, TNF-α and IL-36 in response to environmental stressors in genetically susceptible individuals
- Activated dendritic cells release IL-23 which activates T cells and innate lymphoid cells
- Activated T cells and innate lymphoid cells release TNF-α, IL-17 and IL-22 to promote keratinocyte hyperproliferation, neutrophil recruitment and chemokine production
The psoriatic state is maintained by the differentiation of naïve T cells into Th17 and Th1 cells that migrate to the skin to produce cytokines (IFNγ, IL-17 and IL-22) that promote epidermal cell proliferation, thereby perpetuating the response.
Figure 1. The key cells, cytokines and chemokines involved in initiating and perpetuating the psoriatic state.
CCL20, chemokine ligand 20; CCR6, chemokine receptor 6; CLA, cutaneous lymphocyte antigen; CXCL, chemokine (C-X-C motif) ligand; IFN-γ, interferon-gamma; IL, interleukin; ILC, innate lymphoid cells; PRRs, pattern recognition receptors; RORγt, retinoid-related orphan receptor γt; TH, T helper cell; TNF-α, tumour necrosis factor-alpha.
Biologic treatments for moderate-to-severe psoriasis
In the last 15 years, biologic treatments that are based on disease pathophysiology have provided targeted treatment options for patients with moderate-to-severe psoriasis. These biologics are antibodies that bind to and inhibit one or more factors involved in psoriasis initiation and maintenance:
- TNF-α inhibitors: etanercept, infliximab, adalimumab, certolizumab pegol
- IL-12/IL-23 inhibitors: ustekinumab
- IL-17 inhibitors: secukinumab, ixekizumab, brodalumab
- IL-23 inhibitors: guselkumab, tildrakizumab, risankizumab
Figure 2. Timeline for European Medicines Agency (EMA) approval of different treatments for psoriasis.
Importantly, some of the biologic treatments are used to treat other autoimmune diseases. For instance, the TNF-α inhibitor, certolizumab pegol, was approved for the treatment of moderate-to-severe plaque psoriasis in 2018, however was first indicated for Crohn’s disease in 2008 and is also used to treat rheumatoid arthritis and ankylosing spondylitis.
Unmet needs in psoriasis
Some of the key unmet needs for psoriasis relates to identifying patients who need systemic treatments, selecting the right treatment for the patient and setting attainable treatment goals. Treatment selection should be based on a balance of treatment efficacy, safety, tolerability and likelihood of adherence. This balance can vary for different patient populations, for example those with comorbidities or those who have safety concerns related to family planning.
Figure 3. Overview of unmet needs in psoriasis.
Currently, biologic treatments all provide much better efficacy compared to placebo and are relatively equivalent when compared to each other. However, each biologic has distinct features that may be beneficial for different patient groups. Key differences can involve:
- Initial speed of clearance
- Ability to achieve long-term disease control
- Adverse events and availability of long-term safety data
- Indication for comorbidities such as psoriatic arthritis
For example, a wealth of safety data for TNF-α inhibitors is now available from multiple clinical trial studies, patient registries and other indications, allowing the physician to make a well-informed decision on safety when prescribing this biologic. This is particularly important for a patient group with heightened concerns surrounding safety, such as women who are planning a family and are often omitted from clinical trials. For this reason, it may not be advisable to treat a young woman with a biologic for which safety data gathered during pregnancy and breast-feeding was not available.
A major unmet need in psoriasis is therefore in understanding how to stratify patients to the right treatments.
Part 2: Treating moderate-to-severe psoriasis in women who are of child-bearing age.
Part 3: Considering differences in the evidence base for moderate-to-severe psoriasis treatments.
Further reading
Gottlieb AB, Ryan C, Murase JE. Clinical considerations for the management of psoriasis in women. Int J Womens Dermatol. 2019;5:141–150.
Schadler ED, Ortel B, Mehlis SL. Biologics for the primary care physician: Review and treatment of psoriasis. Dis Mon. 2019;65:51–90.