Earlier enzyme therapy reshapes Pompe outcomes
By Laura Boyd
Early initiation of enzyme replacement therapy (ERT) in children with late‑onset Pompe disease (LOPD) identified through newborn screening (NBS) may improve motor outcomes and stabilize disease progression, according to data from WORLDSymposium 2026 (We’re Organizing Research on Lysosomal Diseases).
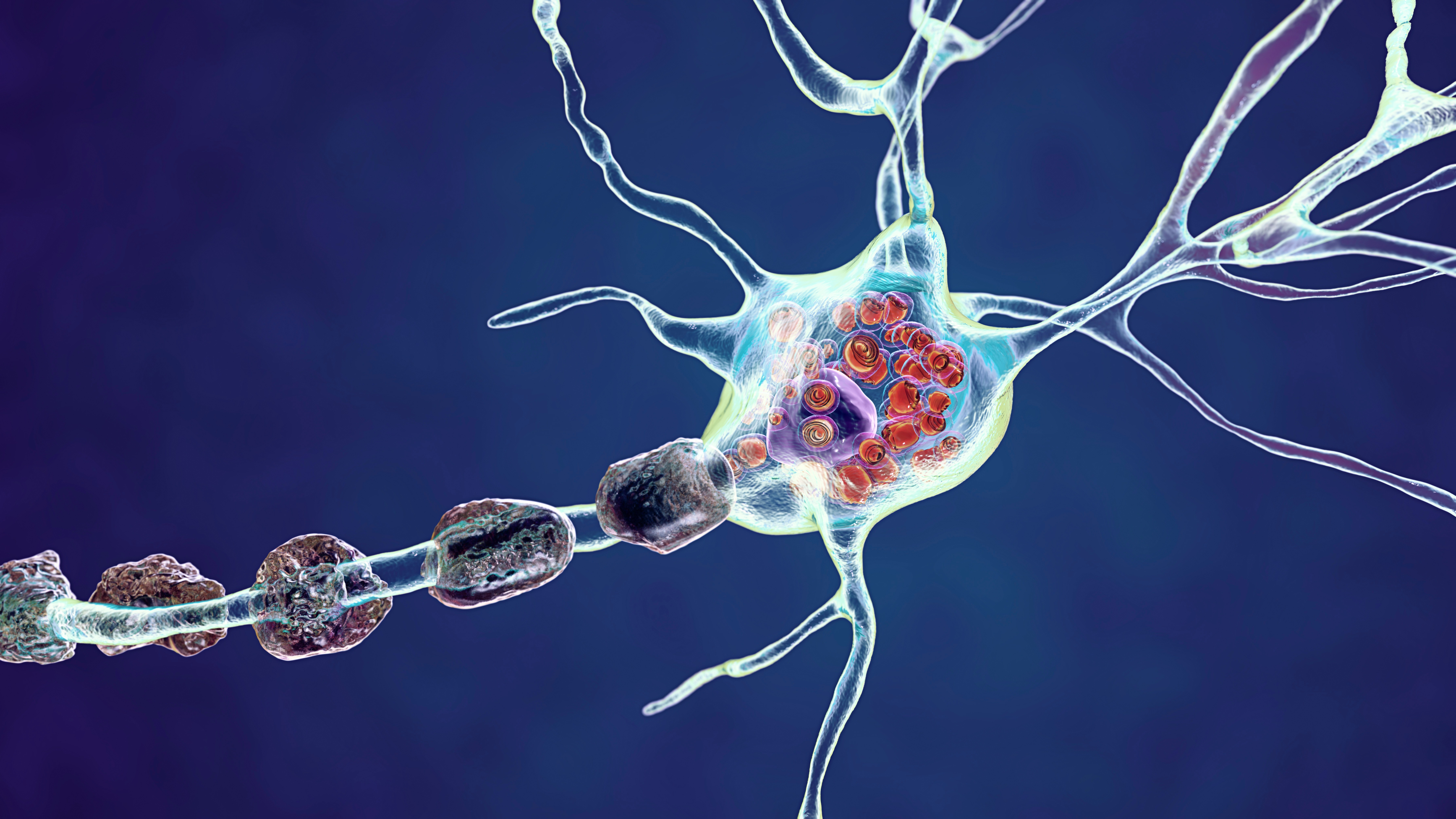
Laura Case (Duke University, Durham, North Carolina, USA) reported early ERT outcomes from seven symptomatic children with LOPD diagnosed through NBS, demonstrating that clinically meaningful disease manifestations can emerge within the first year of life. All patients carried the common IVS1 (c.-32‑13T>G) variant alongside a second pathogenic or likely pathogenic variant. Before treatment, all patients exhibited postural and kinematic abnormalities and persistently elevated creatine kinase (CK), with 86% showing standardized gross motor scores at or below the 10th percentile or evidence of decline. Based on these findings, the authors note that “kinematic abnormalities may precede declines on standardized gross motor testing.”
Patients initiated ERT at a median age of 8.2 months, beginning with alglucosidase alfa and later transitioning to avalglucosidase alfa, without reported complications. At latest follow‑up, all children demonstrated significant improvements in motor function alongside normalization of CK levels. Quantitative muscle ultrasound findings supported these clinical improvements, with reduced muscle echo‑intensity observed over time. Case emphasized that comprehensive, multidisciplinary evaluation – including physical therapy‑led kinematic assessment, standardized motor testing, speech and feeding evaluation, and biomarker monitoring – is important, “allowing timely intervention for those that may benefit from early ERT.”
Complementary findings presented by KeriAnn Kuperman (Children’s National Hospital, Washington, DC, USA) compared the clinical trajectories of patients diagnosed before and after NBS implementation. Drawing on 8 years of regional screening data, Kuperman reported that NBS identified approximately 50 times more infants at risk for LOPD than infantile‑onset Pompe disease, often without clear genotype–phenotype correlations or symptoms at diagnosis.
Among two adults diagnosed before NBS, symptom onset occurred at a mean age of 2.5 years, with ERT initiated over 2 decades later. Both showed advanced disease, including impaired pulmonary function, gait abnormalities, reduced 6‑minute walk distances, and skeletal complications such as osteoporosis.
In contrast, two children identified through NBS presented with symptomatic disease in infancy and initiated ERT at a mean age of 13.5 months, with markedly elevated biomarkers before treatment initiation. Now aged 6 and 5.5 years, both demonstrate preserved respiratory function, no functional impairment, and objective improvements in gross motor performance. Kuperman concluded that “early identification provides an opportunity to alter the progression trajectory for LOPD… transforming what would otherwise be a slow decline to a more stable long-term course with preserved independence...”
Together, these data highlight that NBS enabled timely treatment. The presenters conclude that structured, longitudinal monitoring may help identify patients most likely to benefit from early enzyme therapy.
Read more about early biomarkers and symptoms in NBS-identified LOPD.
Developed by EPG Health for Medthority, independently of any sponsor.